


Understanding angina is essential, particularly for older adults, as chest pain can present itself in various ways, often leading to confusion and misdiagnosis. This article explores vital self-care strategies that empower seniors to manage their condition effectively, from recognizing symptoms to making lifestyle changes.
Yet, a significant challenge persists: how can elderly patients navigate the complexities of angina management while ensuring they receive the necessary support? Reflecting on this question highlights not only the importance of informed self-care but also the crucial role of healthcare provider engagement in enhancing quality of life. Together, we can foster a supportive environment that encourages proactive health management.
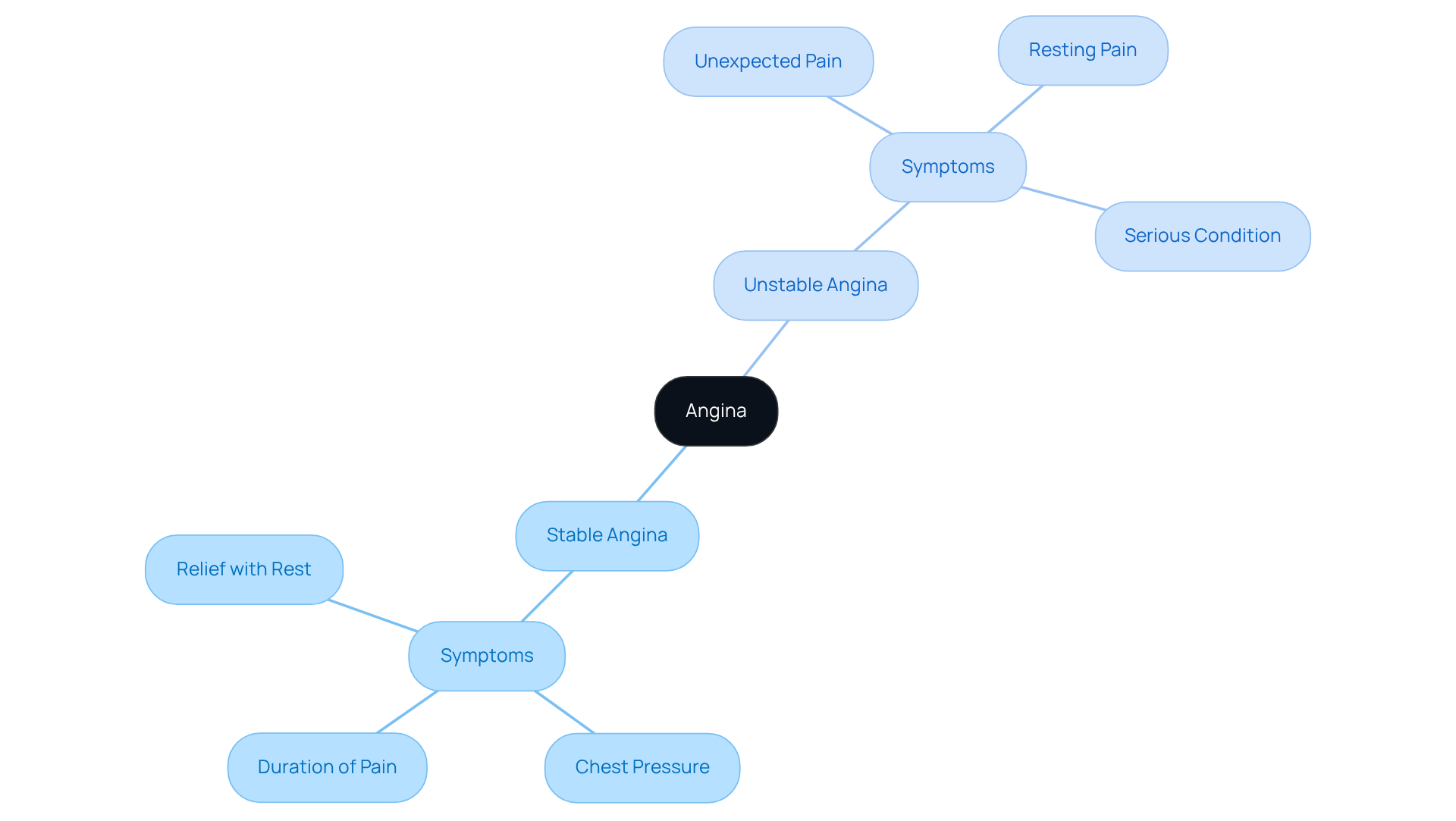
, a type of discomfort that can arise from decreased blood flow to the heart, is categorized into two main forms: stable and unstable. typically occurs during physical exertion or emotional stress, but it can be relieved with rest or medication. Patients often describe this sensation as pressure, squeezing, or heaviness in the chest, lasting anywhere from 2 to 10 minutes. On the other hand, unstable may strike unexpectedly, even at rest, and can signal a more serious condition that requires immediate medical attention.
For older individuals, the experience of is particularly noteworthy, with stable forms being more common. However, many elderly patients might face atypical symptoms, such as shortness of breath, excessive fatigue, or discomfort resembling indigestion, which can complicate diagnosis and management. Importantly, angina can manifest even without significant coronary blockages, leading to potential misunderstandings about its implications. This situation is concerning, as can limit daily activities and heighten the risk of cardiac arrest.
Understanding these variations is vital for effective . Cardiologists at Amavita emphasize the importance of recognizing both to ensure timely intervention. Our specialists are dedicated to using advanced diagnostic imaging to identify blockages and offer minimally invasive procedures, like and stent placement, to restore blood flow. As one expert thoughtfully remarked, 'A thorough medical history is essential for diagnosing chest pain, often requiring objective tests for confirmation.' This highlights the necessity for elderly patients to remain vigilant about their symptoms and to communicate openly with their healthcare providers to .
Additionally, it is essential to consider the impact of , which can lead to palpitations and fatigue, in relation to chest pain. This underscores the importance of being aware and proactive in managing one’s health. Remember, you are not alone in this journey; seeking help and support is a crucial step towards maintaining your .
Making lifestyle adjustments can greatly improve angina self-care and control of chest pain in older adults. It's important to explore some key strategies that can help you feel better and live a healthier life.
By embracing these , you can take proactive steps towards angina self-care, effectively managing your condition and ultimately improving your quality of life. For instance, a study on the effects of lifestyle changes in older adults with chest pain demonstrated notable enhancements in their overall well-being and a decrease in episodes of discomfort, emphasizing the real benefits of these approaches. Remember, you are not alone in this journey, and can make a significant difference.

Medications play a crucial role in managing , especially for older adults who may feel anxious about their health. Understanding the options can help provide some peace of mind. Here are some key medications that can offer relief:
is crucial for effective management of chest pain. It’s important for patients to maintain about any side effects or concerns, ensuring their treatment plan is tailored to their health needs. Additionally, remember that nitrates should not be combined with certain medications, such as phosphodiesterase inhibitors, due to the risk of severe hypotension. By staying informed and engaged with your healthcare team, you can take proactive steps towards better through angina self-care.

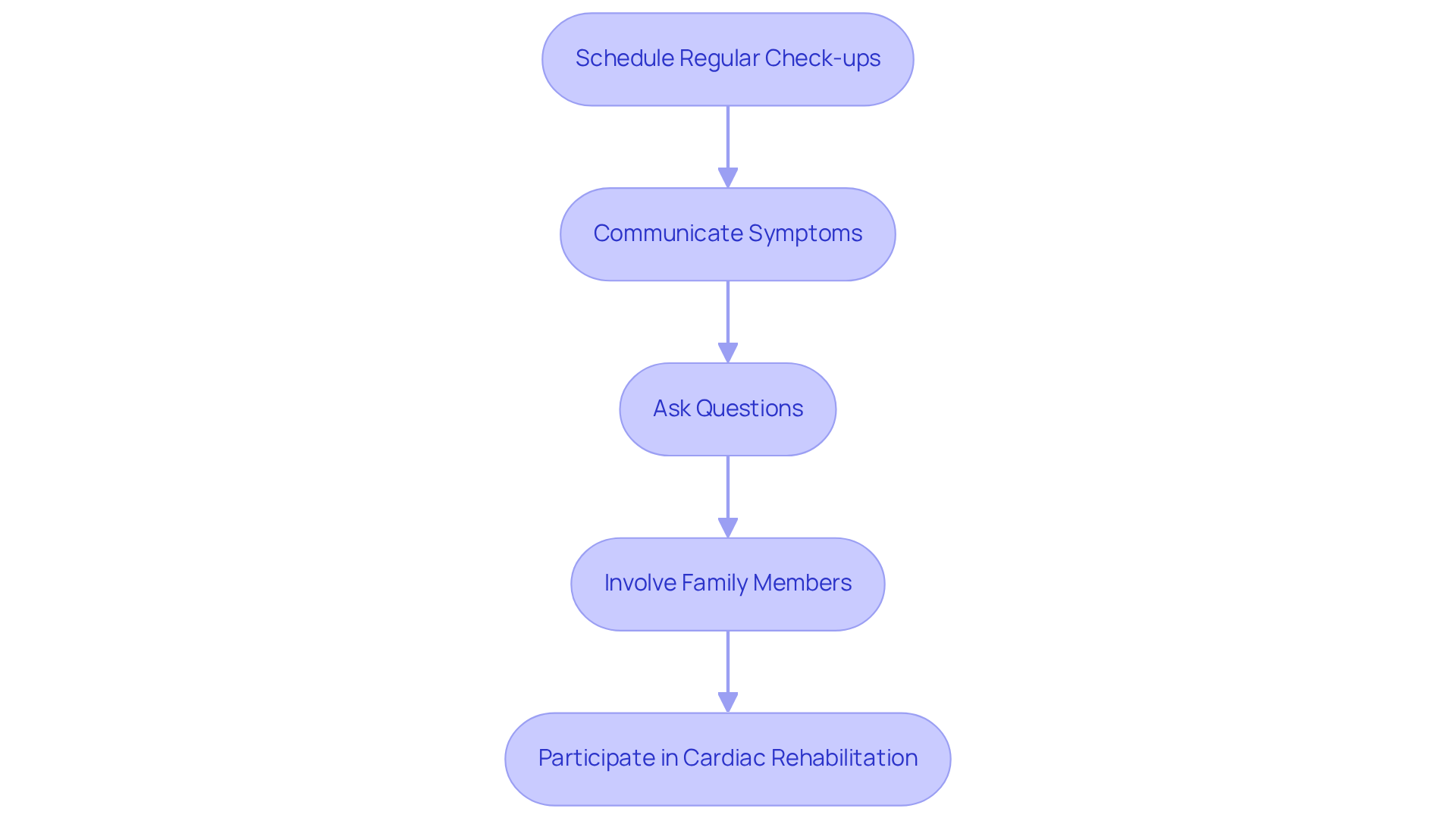
Engaging with healthcare providers is vital for . At Amavita Heart and Vascular Health, we emphasize the importance of proactive patient involvement in care, especially for those at high risk. Here are some steps to enhance communication and involvement:
Real-world examples illustrate that effective patient-provider communication can significantly enhance angina self-care management outcomes. For instance, individuals who actively share their experiences and concerns often report improved symptom management and overall satisfaction with their care. Engaging healthcare providers in this manner not only enhances treatment efficacy but also empowers individuals to take charge of their .
As one patient noted, "When I think about it, it is when I’m depressed that I eat stuff I shouldn’t and drink too much. … I just want to feel better, I just want to get to some kind of normal life." This highlights the importance of open communication in addressing not just physical symptoms but also emotional well-being.
Understanding and managing angina is crucial for elderly patients, as it directly impacts their overall heart health and quality of life. By recognizing the symptoms and types of angina—stable and unstable—older adults can take proactive steps in their self-care journey. This awareness is essential not only for timely medical intervention but also for fostering effective communication with healthcare providers, which is vital for tailored treatment plans.
The article outlines several key strategies for managing angina. These include lifestyle modifications such as:
Furthermore, it emphasizes the importance of medication adherence and regular check-ups with healthcare professionals. Collectively, these measures empower older adults to take charge of their health, mitigating the risks associated with angina and enhancing their overall well-being.
Ultimately, the journey toward effective angina self-care is a shared responsibility that involves both the patient and their healthcare team. By actively participating in their treatment and embracing lifestyle changes, elderly patients can significantly improve their heart health and quality of life. Encouraging open dialogue with healthcare providers and seeking support from family can further enhance this process. This ensures that individuals feel empowered and informed in managing their condition.
What are the two main types of angina?
The two main types of angina are stable angina and unstable angina. Stable angina occurs during physical exertion or emotional stress and can be relieved with rest or medication, while unstable angina can occur unexpectedly, even at rest, and may indicate a more serious condition.
How do patients typically describe stable angina?
Patients often describe stable angina as a sensation of pressure, squeezing, or heaviness in the chest, lasting anywhere from 2 to 10 minutes.
What are atypical symptoms of angina in older individuals?
Atypical symptoms of angina in older individuals may include shortness of breath, excessive fatigue, or discomfort resembling indigestion, which can complicate diagnosis and management.
Can angina occur without significant coronary blockages?
Yes, angina can manifest even without significant coronary blockages, which may lead to misunderstandings about its implications and the severity of the underlying condition.
Why is it important for elderly patients to recognize their symptoms?
It is important for elderly patients to recognize their symptoms to ensure timely intervention and effective management of their heart health, as they may experience atypical signs.
What role do cardiologists play in managing angina?
Cardiologists use advanced diagnostic imaging to identify blockages and offer minimally invasive procedures, such as cardiac catheterization and stent placement, to restore blood flow.
What is the significance of a thorough medical history in diagnosing chest pain?
A thorough medical history is essential for diagnosing chest pain and often requires objective tests for confirmation to ensure accurate diagnosis and appropriate treatment.
How do arrhythmias relate to chest pain?
Arrhythmias can lead to palpitations and fatigue, which underscores the importance of being aware and proactive in managing one’s health in relation to chest pain.