


Heart failure is a complex and often daunting condition that affects millions, particularly the elderly, who face unique challenges in managing their health. As research continues to evolve, the landscape of heart failure medications is expanding, offering new hope for improved outcomes and quality of life. This article delves into ten essential heart failure medications that not only enhance treatment efficacy but also emphasize the importance of personalized care strategies.
With so many options available, how can patients and caregivers navigate this intricate web of therapies to find the most effective solutions for their specific needs? We understand that this journey can feel overwhelming, but you are not alone in seeking the best care.
At Amavita Heart and Vascular Health, we are wholeheartedly dedicated to providing comprehensive treatment management for individuals facing cardiac issues, particularly our elderly patients, who often encounter unique challenges in their care. By emphasizing patient-centered care, we seamlessly integrate state-of-the-art treatments with compassionate support. Our skilled team is committed to ensuring that each patient receives medications that specifically address their health needs, ultimately enhancing adherence and improving outcomes.
Our effective programs for managing cardiac dysfunction highlight the importance of early intervention. Research indicates that utilizing evidence-based therapies can significantly improve heart failure outcomes, reducing hospital visits and enhancing quality of life. As we look toward optimal approaches for 2025, we emphasize regular reviews of medications, lifestyle changes, and close monitoring of treatment responses—essential elements for successful management.
Amavita proudly offers advanced treatment options, including minimally invasive valve repairs and catheter-based interventions, allowing individuals to return home the same day. Our cardiologists advocate for a client-focused strategy, underscoring that individualized care is crucial for elderly individuals dealing with heart failure. As one expert wisely noted, "Customizing treatment to the individual not only enhances adherence but also empowers individuals in their health journey." This philosophy is at the heart of Amavita's approach, ensuring that every patient receives the attention and care they truly deserve in their recovery. Additionally, we collaborate with Jackson Memorial and Mercy Hospitals to further enhance the quality of care we provide.
ACE inhibitors, such as lisinopril and ramipril, play a vital role in managing heart failure, addressing a concern many may have about their health. By inhibiting the angiotensin-converting enzyme, these medications promote vasodilation and lower blood pressure, which in turn reduces the workload on the heart and enhances cardiac output. Clinical studies have shown that these medications significantly lower hospitalization rates and mortality among individuals with heart failure, providing hope for better health outcomes.
For instance, the PARADIGM-HF trial revealed that LCZ696, a new treatment option, decreased hospitalization rates compared to traditional medications like enalapril. This finding is particularly encouraging for older individuals, as studies have demonstrated a benefit within this group. Regular use of ACE inhibitors is associated with improved symptoms and an overall enhancement in quality of life, making them essential components of treatment for those at risk.
Furthermore, recent research indicates that ACE inhibitors, including drugs such as lisinopril and ramipril, not only improve survival rates but also help enhance functional capacity in individuals with heart failure. In the context of Amavita's care model, these treatments are crucial in addressing the [cardiovascular challenges](https://amavita.health/blog/understanding-cardioversion-for-atrial-fibrillation-a-patients-guide) faced by skilled nursing facilities, including high readmission rates and care coordination issues. This approach has contributed to a remarkable 93% reduction in readmissions and significant cost savings, ultimately enhancing patient outcomes through advanced diagnostic tools and seamless care coordination.
If you or a loved one are navigating these challenges, know that there are resources available, and support is always within reach. Your health matters, and together, we can work towards a brighter, healthier future.
For many individuals facing challenges with heart failure, medications such as losartan and valsartan offer a compassionate alternative. These medications work by inhibiting the effects of angiotensin II, promoting vasodilation, and ultimately helping to improve blood flow. This is crucial for managing symptoms. Recent studies have shown that medications such as ARBs can significantly improve outcomes, particularly in patients with preserved ejection fraction.
However, it’s important to approach their use with care. A meta-analysis involving over 25,000 individuals indicated that ARB therapy did not significantly reduce total mortality or hospitalizations compared to placebo. This finding underscores the need for thoughtful consideration when choosing treatment options. In practice, ARBs are often recommended for individuals who experience side effects from ACE inhibitors, as they tend to be better tolerated.
Yet, combining ARBs with other medications may increase the risk of withdrawals due to adverse effects, without offering benefits in reducing total mortality or hospital admissions. While ARBs like losartan and valsartan have their advantages, ACE inhibitors should still be viewed as the primary treatment due to their effectiveness in lowering mortality and morbidity in patients with cardiac issues.
Ultimately, the choice between ARBs and ACE inhibitors should be guided by individual responses and tolerability. This ensures that each patient receives the most appropriate care for managing their heart failure. Remember, you are not alone in this journey; reaching out for support can make a significant difference in your health and well-being.

Beta blockers play a vital role in managing cardiac dysfunction, especially for our elderly loved ones. They work by gently lowering the pulse rate and reducing the heart's oxygen needs, which is crucial for those facing heart failure. Studies have shown that these medications can significantly improve heart function, particularly those with a lower ejection fraction. This is especially beneficial for older adults, who often experience fatigue and increased cardiac strain.
Through Amavita's heart health program, we are dedicated to transforming patient care. By implementing advanced diagnostic tools and promoting seamless coordination among caregivers, we have achieved an impressive 93% reduction in readmissions. This program not only addresses the cardiovascular challenges faced by skilled nursing facilities but also enhances the overall health outcomes for our elderly residents. We are committed to ensuring that they receive the care they truly deserve.
If you or a loved one is navigating the complexities of heart disease, know that support is available. We understand the concerns that come with cardiac issues, and we are here to provide the resources needed to improve quality of life. Together, we can make a difference in your journey towards better health.
Diuretics, such as furosemide and torsemide, are essential medications that help individuals manage fluid retention, particularly among the elderly population. These medications assist in the excretion of excess fluid through the kidneys, providing relief from uncomfortable symptoms such as swelling and shortness of breath. However, it's important to approach their use with care, as older adults may face complications such as electrolyte imbalances and dehydration. Recent clinical evidence highlights the need for careful monitoring, as long-term diuretic use has been associated with a concerning 31% increase in hospitalizations in this group.
Healthcare professionals emphasize that while diuretics are vital for alleviating symptoms, it’s worth reconsidering their regular use in individuals who are asymptomatic or only mildly symptomatic. As one expert wisely noted, "Clinicians might also consider adding low-dose digoxin, instead of increasing the dose of diuretics, to improve heart function." Thus, ongoing monitoring and individualized care are crucial in ensuring the best possible outcomes for elderly individuals facing heart failure. Remember, you are not alone in this journey; with support and confidence.
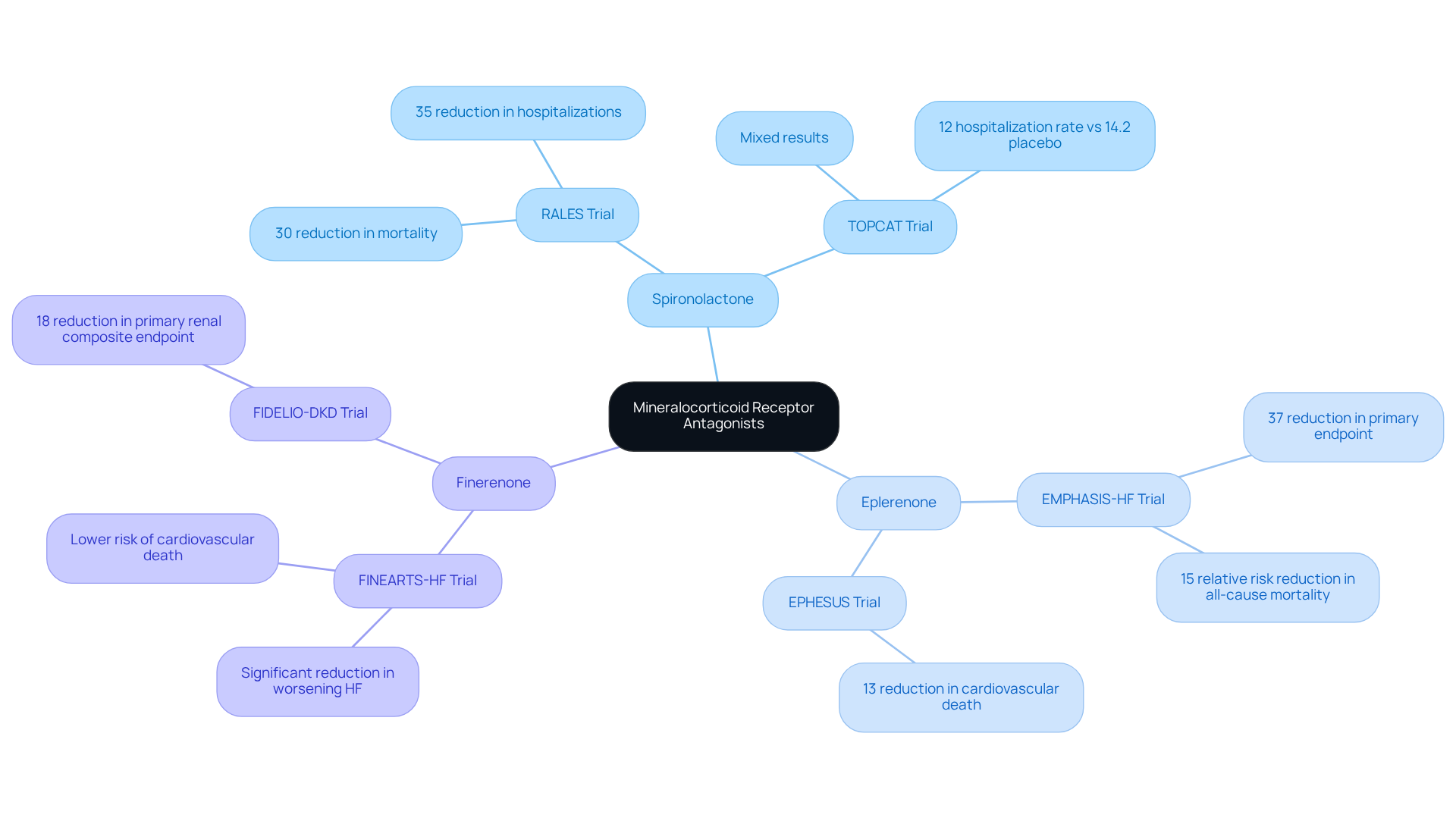
Mineralocorticoid Receptor Antagonists (MRAs), such as spironolactone and eplerenone, have become recognized as vital components in managing [heart failure](https://amavita.health/blog/10-effective-treatments-for-chf-to-improve-your-heart-health). These medications work by blocking the effects of aldosterone, a hormone that can cause fluid retention and harmful changes in the heart, ultimately facing these challenges. Recent studies highlight how MRAs can significantly improve outcomes, especially for patients with reduced ejection fraction (HFrEF). For instance, the RALES trial showed that spironolactone therapy resulted in a 30% relative decrease in mortality and a 35% drop in hospitalizations due to worsening heart conditions. Similarly, the EMPHASIS-HF trial revealed that eplerenone lowered the primary endpoint by 37%, reinforcing its effectiveness in alleviating symptoms.
In addition to this, the FINEARTS-HF trial examined finerenone, a newer non-steroidal MRA, in patients with heart failure with preserved ejection fraction (HFpEF) and mildly reduced ejection fraction (HFmrEF). This trial demonstrated that finerenone significantly lowered the risk of [hospitalization and cardiovascular events](https://amavita.health/blog/10-essential-atrial-fibrillation-news-updates-you-should-know), highlighting its potential benefits across various cardiac profiles. Overall, MRAs have shown a remarkable ability to reduce mortality, with a pooled hazard ratio of 0.77 for cardiovascular mortality or cardiac hospitalization. This establishes them as a cornerstone in managing [cardiac issues](https://amavita.health/blog/10-gae-patient-reviews-near-me-real-experiences-and-insights). As our understanding of MRAs continues to evolve, their integration into treatment plans is expected to enhance the management of cardiac challenges, offering hope and support for a better future.
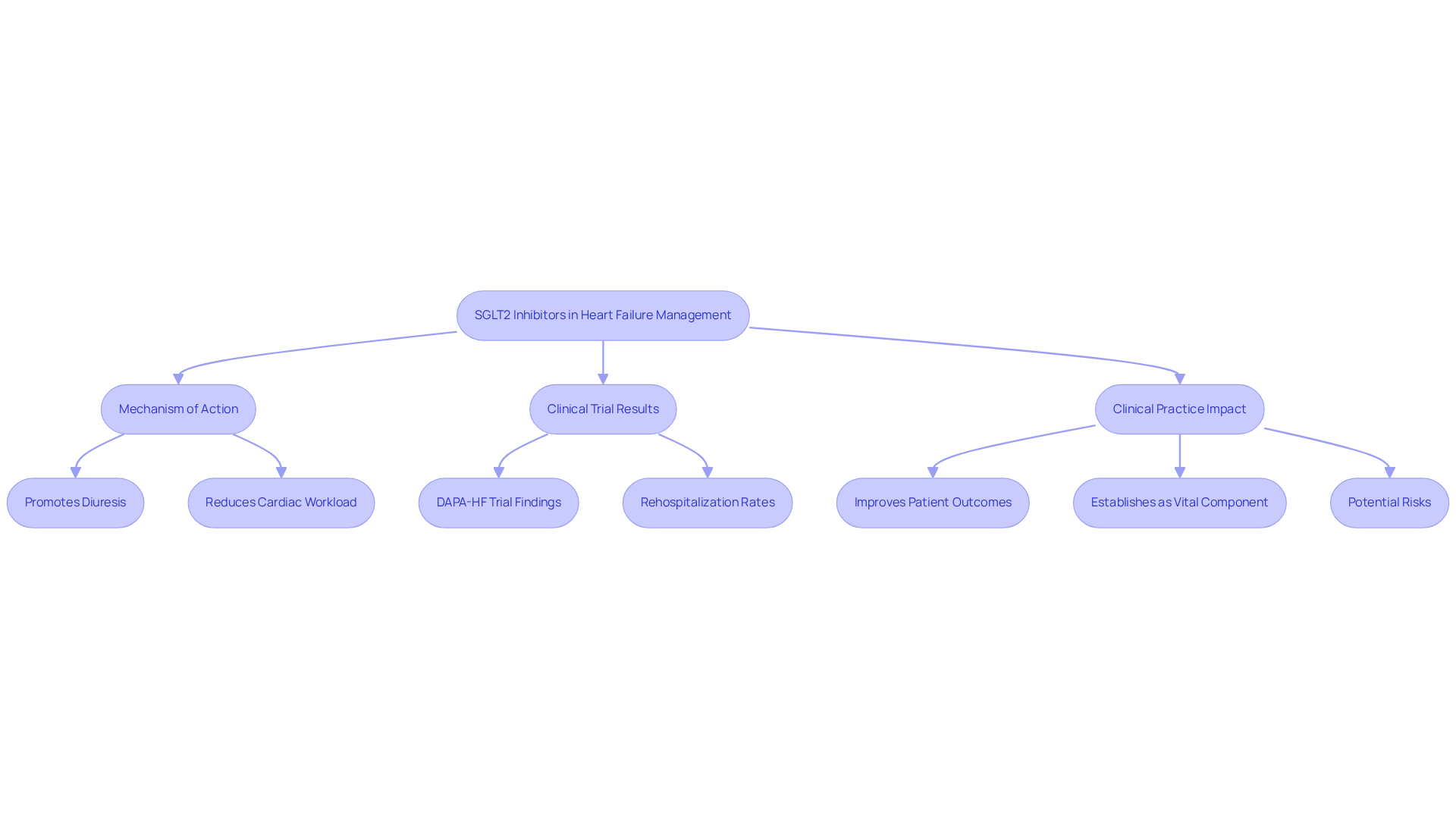
SGLT2 inhibitors, including empagliflozin and dapagliflozin, have emerged as transformative options in managing heart failure. Initially developed for diabetes, these medications have shown remarkable efficacy, significantly reducing cardiac hospitalizations and improving renal outcomes. Their mechanism of action promotes diuresis, alleviating fluid overload and decreasing cardiac workload, which is crucial for individuals facing heart failure.
Recent studies underscore the effectiveness of SGLT2 inhibitors in enhancing patient outcomes. For instance, the DAPA-HF trial revealed that dapagliflozin reduced hospitalization and mortality in patients with reduced ejection fraction (HFrEF). Specifically, cardiovascular death or worsening heart failure occurred in 10.9% of the dapagliflozin group compared to 12.7% in the placebo group, showcasing a weighted hazard ratio of 0.75. This indicates a 25% lower risk of death among those using dapagliflozin.
Furthermore, dapagliflozin has been shown to significantly decrease hospitalization rates. In a recent analysis, hospitalization was 22.3% for patients treated with dapagliflozin during their hospital stay, compared to 44.4% for those who began treatment after discharge. This suggests that early intervention with SGLT2 inhibitors can lead to better outcomes.
Experts highlight the importance of these medications in routine clinical practice. As noted by Prof. Vass Vassiliou, SGLT2 inhibitors not only reduce hospitalizations due to cardiac issues but also improve overall health, establishing them as a vital component of heart failure management. However, it is essential to be aware of potential risks associated with SGLT2 inhibitors, such as symptomatic hypotension and worsening renal function, to provide a balanced perspective on their use. Incorporating these medications into treatment plans represents significant progress in managing cardiovascular conditions, especially for individuals with concurrent diabetes or kidney problems.
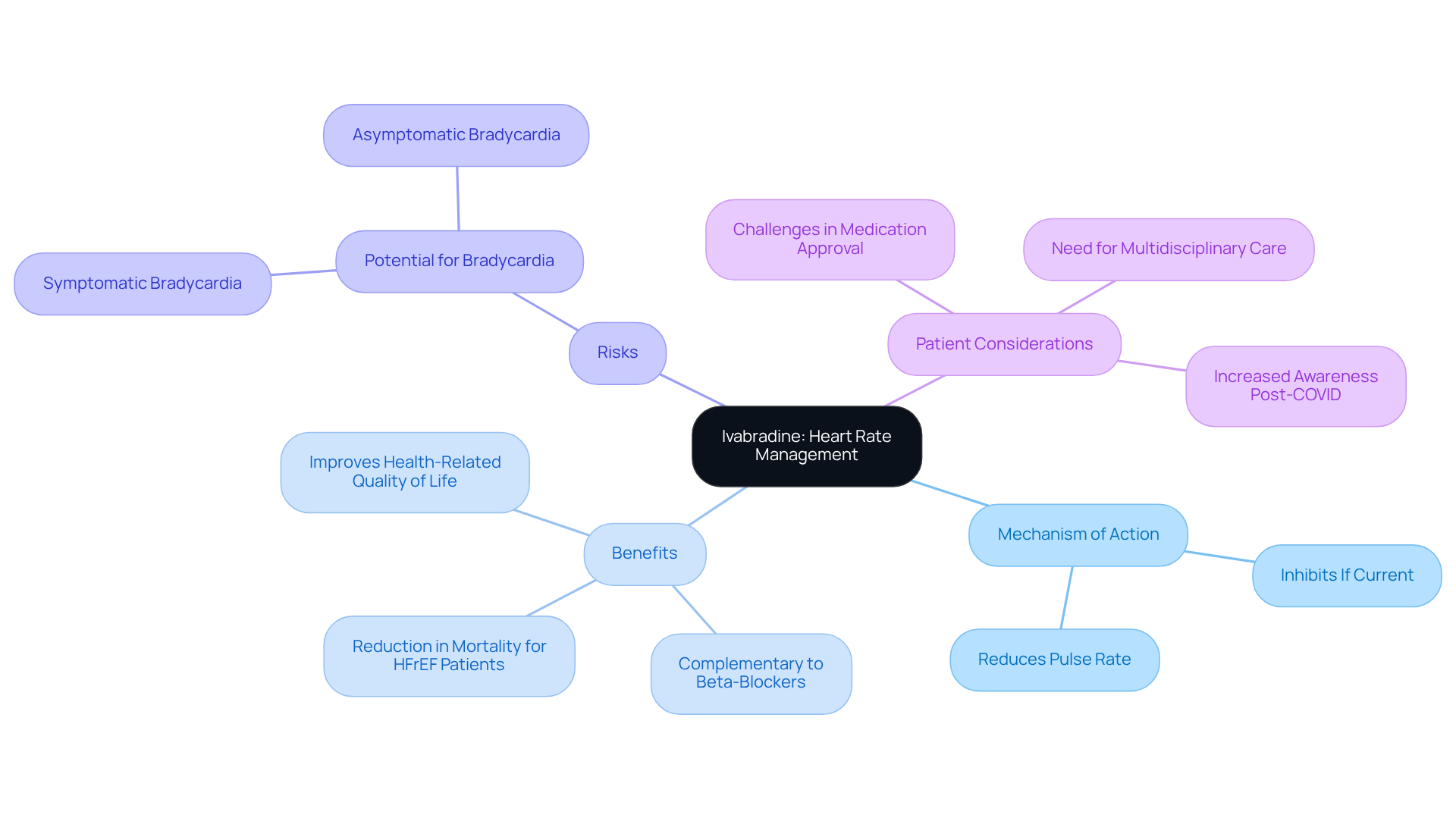
Ivabradine is a unique medication that plays a vital role in heart failure treatment, particularly for those experiencing elevated heart rates. By selectively inhibiting the If current in the sinoatrial node, it effectively reduces pulse rate without affecting blood pressure. This makes ivabradine a valuable option for individuals who still experience symptoms despite receiving standard heart failure therapies, providing an additional strategy for effectively managing heart failure.
Recent observational studies have shown that ivabradine is associated with improved outcomes for individuals with reduced ejection fraction (HFrEF). Given that approximately 64 million people around the world are affected by cardiac dysfunction, the importance of effective treatment options cannot be overstated. While the benefits of ivabradine are substantial, it is essential to be aware of the potential side effects, an important consideration for ensuring patient safety.
A recent trial has further assessed the efficacy and safety of ivabradine, reinforcing its importance as a key component of heart failure management, especially for those who find traditional therapies challenging. If you or a loved one are navigating these health concerns, know that support resources are available. Reaching out for help can make all the difference in managing your heart health effectively.
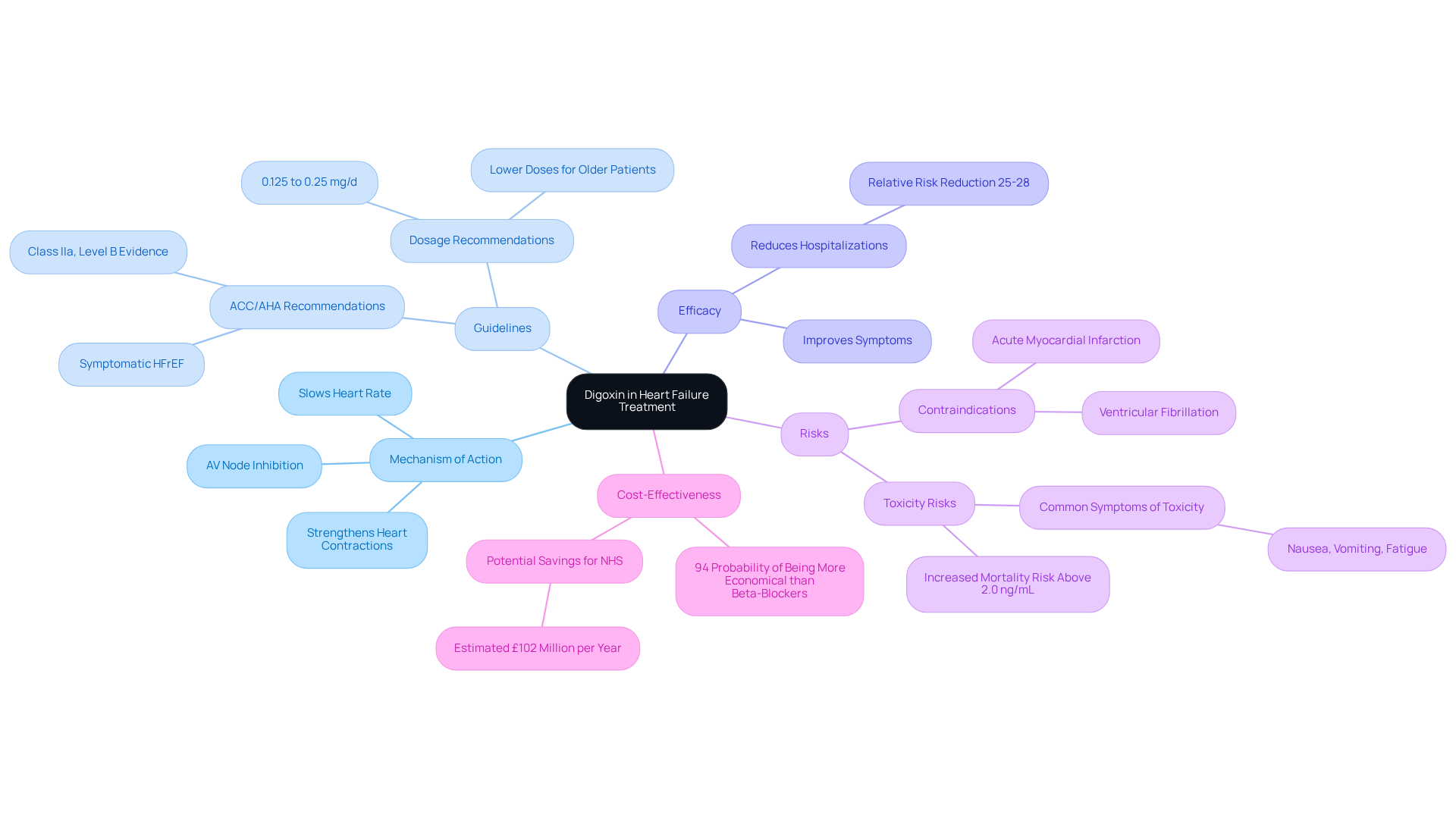
Digoxin, a time-honored medication in managing heart failure, continues to be an important part of modern treatment plans. This cardiac glycoside works by increasing the strength of heart contractions and slowing the heart rate, offering significant benefits for those experiencing cardiac insufficiency and heart rhythm disorders. While newer therapies have emerged, digoxin remains a viable option for individuals who may not respond well to first-line treatments.
It’s crucial to understand that, although digoxin can be effective, it does not reduce mortality rates. Therefore, it should be used cautiously in individuals without heart failure symptoms, as it may lead to worse outcomes. The American College of Cardiology/American Heart Association (ACC/AHA) guidelines recommend digoxin for those with heart failure with reduced ejection fraction (HFrEF), particularly for individuals who continue to experience symptoms despite treatment with neurohormonal antagonists (Class IIa, Level of Evidence B).
Recent studies have shown that digoxin can improve outcomes in individuals with HFrEF, indicating a relative risk reduction of 25-28%. Additionally, its cost-effectiveness is notable, with a 94% probability of being more economical compared to beta-blockers at the standard quality-adjusted life year threshold.
As healthcare professionals, it is essential to navigate the complexities of treatment with diligence and care. Understanding digoxin's pharmacology, its potential risks, including toxicity, and its role in managing heart failure is vital for optimizing outcomes for our patients. We are here to support you and ensure that you receive the best possible care tailored to your needs.
Customized drug management is vital for enhancing cardiovascular treatment, particularly for older individuals who may have multiple health issues. By taking into account individual traits such as age, comorbidities, and specific types of heart failure, healthcare providers can create treatment plans that not only improve efficacy but also minimize side effects. This tailored approach has shown significant improvements in clinical outcomes. For instance, individuals utilizing personalized strategies have experienced remarkable advancements in their treatment management without an increase in hospital admissions or emergency visits.
Furthermore, research indicates that nearly half of U.S. counties lack a cardiologist, underscoring the need for scalable solutions that can reach individuals in underserved areas. Healthcare professionals emphasize that personalized care can lead to longer lives and fewer hospitalizations, reinforcing the commitment to compassionate care, exemplified by Amavita. By prioritizing individualized treatment, we can enhance the quality of life for patients, ensuring they receive the best possible care.
Are you or a loved one feeling uncertain about your heart health? Remember, you are not alone, and there are dedicated professionals ready to support you. Together, we can navigate challenges and find the best path forward.

Effective management of heart failure relies on integrating personalized medication strategies that meet the unique needs of each patient. By taking a comprehensive approach, healthcare providers can significantly enhance outcomes for individuals facing cardiac challenges, especially within the elderly population. Emphasizing tailored treatment plans, the importance of adherence, and continuous monitoring of responses makes the potential for improved quality of life and reduced hospitalizations a tangible reality.
This article has explored a variety of heart failure medications, such as ACE inhibitors, ARBs, beta blockers, diuretics, MRAs, SGLT2 inhibitors, ivabradine, and digoxin. Each medication plays a crucial role in addressing specific aspects of heart failure, from managing fluid retention to improving heart function and reducing mortality rates. As advancements continue to emerge, the significance of personalized care becomes increasingly evident, particularly in optimizing treatment plans for diverse patient profiles.
Ultimately, the journey toward better heart health involves collaboration between patients and healthcare professionals, fostering an environment of support and education. Individuals are encouraged to seek guidance and explore their treatment options, ensuring they are not alone in navigating their health challenges. As the landscape of heart failure management evolves, embracing personalized medication management will remain essential in achieving improved health outcomes and empowering patients on their road to recovery.
What is the focus of Amavita Heart and Vascular Health?
Amavita Heart and Vascular Health is dedicated to providing comprehensive treatment management for individuals facing cardiac issues, particularly elderly patients, by emphasizing advanced therapies and personalized care.
How does Amavita ensure effective management of heart failure?
Amavita emphasizes personalized treatment approaches, regular reviews of heart failure medication, client education, and close monitoring of treatment responses to improve therapy in older adults.
What outpatient procedures does Amavita offer?
Amavita offers advanced outpatient procedures, including minimally invasive valve repairs and catheter-based interventions, allowing individuals to return home the same day.
What role do ACE inhibitors play in heart failure treatment?
ACE inhibitors, such as lisinopril and ramipril, help manage cardiac dysfunction by promoting vasodilation, lowering blood pressure, reducing the workload on the heart, and enhancing cardiac output.
What are the benefits of using ACE inhibitors?
Clinical studies show that ACE inhibitors significantly lower hospitalization rates and mortality among individuals with cardiac dysfunction, improving management of cardiac symptoms and quality of life.
What is the significance of the PARADIGM-HF trial?
The PARADIGM-HF trial revealed that LCZ696, a new treatment option, decreased cardiovascular fatalities by 20% compared to traditional ACE inhibitors, highlighting the importance of these medications for older individuals.
What are Angiotensin II Receptor Blockers (ARBs), and how do they function?
ARBs, such as losartan and valsartan, are alternatives to ACE inhibitors that work by inhibiting the effects of angiotensin II, promoting vasodilation, and helping to lower blood pressure.
Are ARBs as effective as ACE inhibitors?
While ARBs can improve outcomes for those with heart failure, studies indicate they do not significantly reduce total mortality or hospitalizations compared to placebo, making ACE inhibitors the primary treatment choice.
What should guide the choice between ARBs and ACE inhibitors?
The choice should be guided by individual responses and tolerability, ensuring that each patient receives the most appropriate care for managing their cardiovascular conditions.