


Waking up to a racing heart can be quite alarming, leaving many of us wondering what might be causing it. Tachycardia, which is when your resting heart rate exceeds 100 beats per minute, can arise from various factors like anxiety, sleep disturbances, or even dehydration. It’s important to understand this condition, as it not only affects your daily life but may also indicate a need for medical attention.
Have you ever thought about whether that fast heart rate upon waking is just a harmless reaction to stress, or could it be a sign of something more serious? Exploring the causes, symptoms, and treatment options can truly empower you to take charge of your heart health. Remember, you’re not alone in this; many people experience similar concerns, and there are ways to find relief and support.
Tachycardia, or a pulse rate over 100 beats per minute while at rest, can be concerning. It often arises from various factors like stress, anxiety, or health issues such as hyperthyroidism or anemia. It’s important to distinguish between normal responses, like those from exercise, and conditions that may need medical attention. For example, a rapid heartbeat can be a common reaction to stress, usually settling down once the stressor is gone. However, if the rapid heartbeat persists, it might indicate a more serious issue, such as arrhythmia or cardiovascular disease, which could lead to severe complications if not addressed. Symptoms like chest pain, fainting, or shortness of breath warrant immediate medical attention.
At Amavita Heart and Vascular Health, our compassionate specialists are here to help. We use advanced diagnostic tools to uncover the causes of tachycardia, including heart rhythm disorders. Our extensive management options and treatment plans aim to restore your body’s natural rhythm, all while ensuring a patient-centered approach that prioritizes your comfort and convenience.
Treatment for a rapid heartbeat may involve:
Understanding these differences is vital, particularly if you experience palpitations, as it may signal the need for further assessment.
If you experience chest pain or discomfort, it could indicate a serious condition, which requires prompt evaluation and care. Remember, you’re not alone in this journey; we’re here to support you every step of the way.

Tachycardia includes several distinct types, each with its own characteristics and implications for health, especially for individuals who may find support, like that offered by Amavita's services.
Understanding these variations in rapid heartbeat is vital for recognizing symptoms and seeking appropriate care. While sinus tachycardia is often benign, other forms like SVT and VT require intervention to prevent serious health risks. This is where Amavita's services can truly make a difference, providing the support and care you deserve.

can be concerning, and they often include:
Waking up with a fast heart rate can feel unsettling. It’s important to understand that several potential causes may contribute to this experience:
Recognizing these triggers is essential for managing your heart health effectively. At Amavita Heart and Vascular Health, we understand that an unmanaged fast heart rate can lead to significant symptoms and a decline in your quality of life. Our specialists are here to provide expert diagnosis and treatment for conditions like rapid heart rate and tachycardia. Techniques such as vagal maneuvers - like lying down or holding your breath - can help reduce heart rate. However, seeking appropriate care is crucial for your long-term health and well-being.

Diagnosing tachycardia can feel overwhelming, but knowledge can empower you. Here’s a gentle overview of the steps involved:
At Amavita Heart and Vascular Health, we’re committed to using innovative AI-powered diagnostic technology. Our portable, FDA-cleared AI ultrasound for bedside care offers real-time guidance for accurate imaging. This means we can intervene early, helping to prevent tachycardia. By integrating these technologies into our comprehensive care plans, we ensure that individuals at high risk - like those with diabetes, hypertension, or a family history of heart disease - receive the targeted support they need.
Dr. Martinez-Clark’s Harvard training and extensive cardiovascular experience further enhance our ability to provide sophisticated care. Understanding these diagnostic steps allows you to take an active role in your healthcare journey, fostering a sense of control and preparedness. When you’re informed about these processes, you can more effectively engage and collaborate with your healthcare team with confidence.

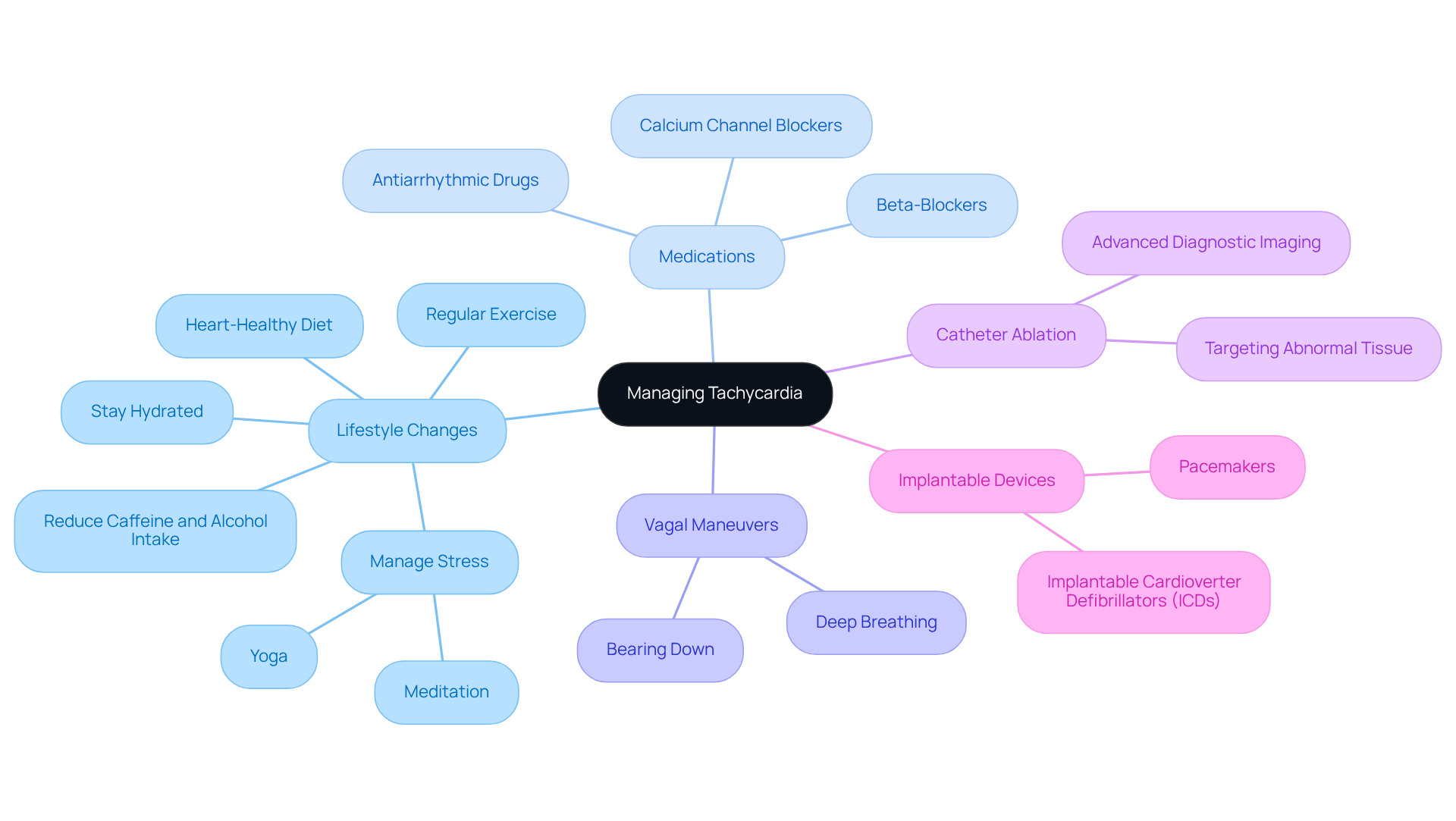
Managing tachycardia effectively requires a thoughtful approach that combines lifestyle changes, medications, and support from healthcare providers.
Understanding these treatment options empowers you to work closely with your healthcare providers at Amavita to create a personalized care plan that meets your unique needs. Together, we can enhance your quality of life and reduce the risks associated with arrhythmias. Remember, you’re not alone in this journey; we’re here to support you every step of the way.
Waking up to a fast heart rate can be unsettling, but understanding what’s happening can help you take control of your heart health. Tachycardia, which means a resting pulse rate over 100 beats per minute, can be caused by various factors like stress, anxiety, or even underlying health issues. It’s important to know the difference between normal responses and more serious concerns so you can decide when to seek medical help.
This article sheds light on different types of tachycardia, including:
Each type has its own characteristics and health implications. If you experience symptoms like palpitations, dizziness, or shortness of breath, it’s a sign that you should get evaluated. The diagnostic process typically involves a thorough review of your medical history, a physical exam, and advanced tests like ECGs and Holter monitors to identify any underlying causes and ensure you receive the right care.
Managing tachycardia effectively requires a well-rounded approach that includes lifestyle changes, medications, and possibly advanced treatments. By prioritizing your heart health and making informed choices, you can significantly enhance your quality of life. Remember, understanding your body and recognizing symptoms is key to proactive management and better cardiovascular health. Taking steps today can lead to a healthier tomorrow.
If you have concerns, don’t hesitate to reach out for support. You’re not alone in this journey, and there are resources available to help you feel better and live well.
What is tachycardia?
Tachycardia is defined as a pulse rate over 100 beats per minute while at rest. It can arise from factors like stress, anxiety, or health issues such as hyperthyroidism or anemia.
What are the common causes of tachycardia?
Common causes include emotional triggers like stress and anxiety, as well as health conditions such as hyperthyroidism and anemia.
When should I seek medical attention for tachycardia?
You should seek medical attention if you experience symptoms like chest pain, fainting, or shortness of breath, as these may indicate a more serious issue.
What treatments are available for tachycardia?
Treatments may involve medications like beta-blockers and calcium channel blockers, lifestyle changes such as reducing caffeine and alcohol intake, managing stress, and maintaining a healthy lifestyle.
What are the different types of tachycardia?
The main types of tachycardia include Sinus Tachycardia, Supraventricular Tachycardia (SVT), Ventricular Tachycardia (VT), and Atrial Fibrillation, each with distinct characteristics and health implications.
What is Sinus Tachycardia?
Sinus Tachycardia is the most common form and is often a normal response to stress, exercise, or anxiety, characterized by a resting pulse exceeding 100 beats per minute.
What is Supraventricular Tachycardia (SVT)?
SVT originates above the ventricles and is marked by sudden episodes of rapid pulse, which can lead to palpitations, dizziness, or shortness of breath. It affects about 2.5 out of every 1000 individuals.
What is Ventricular Tachycardia (VT)?
VT arises from the ventricles and can be life-threatening, potentially leading to severe complications like syncope or cardiac arrest, particularly in individuals with existing cardiovascular issues.
What is Atrial Fibrillation?
Atrial Fibrillation is characterized by an irregular and often rapid heart rate, which increases the risk of blood clots and stroke. Symptoms may include palpitations or fatigue.
How does Amavita's CardioElite™ program assist patients with tachycardia?
The CardioElite™ program offers comprehensive management, advanced diagnostic imaging, and 24/7 cardiology consultation to help identify and manage tachycardia effectively, ensuring patients receive the best care possible.