Introduction
Peripheral Artery Disease (PAD) is a silent yet pervasive condition that affects millions, often going unnoticed until it reveals itself through debilitating symptoms. Did you know that over 12 million people in the United States are grappling with this circulatory disorder? Understanding its causes, symptoms, and treatment options isn’t just beneficial - it’s essential for improving your quality of life.
What if that leg pain you feel during a simple walk is a warning sign of something more serious? It’s important to listen to your body and recognize these signals. Delving into the intricacies of PAD can empower you to take proactive steps toward better health. By being informed, you can make decisions that enhance your care journey.
Remember, you’re not alone in this. Many people share your concerns, and there are resources available to help you navigate this condition. Seeking support can lead to better outcomes and a more fulfilling life. Don’t hesitate to reach out for guidance - your health matters.
Define Peripheral Artery Disease (PAD)
is a common circulatory condition that affects many, particularly in the legs. It occurs when arteries narrow, often due to atherosclerosis, where fatty deposits build up on artery walls, leading to reduced blood flow. In fact, over 12 million individuals in the United States are living with , which makes it a significant .
Many patients experience discomfort, such as leg pain or cramping during physical activities. This can limit mobility and impact overall quality of life. It’s important to recognize that can result in , including a heightened . Understanding this condition is crucial for .
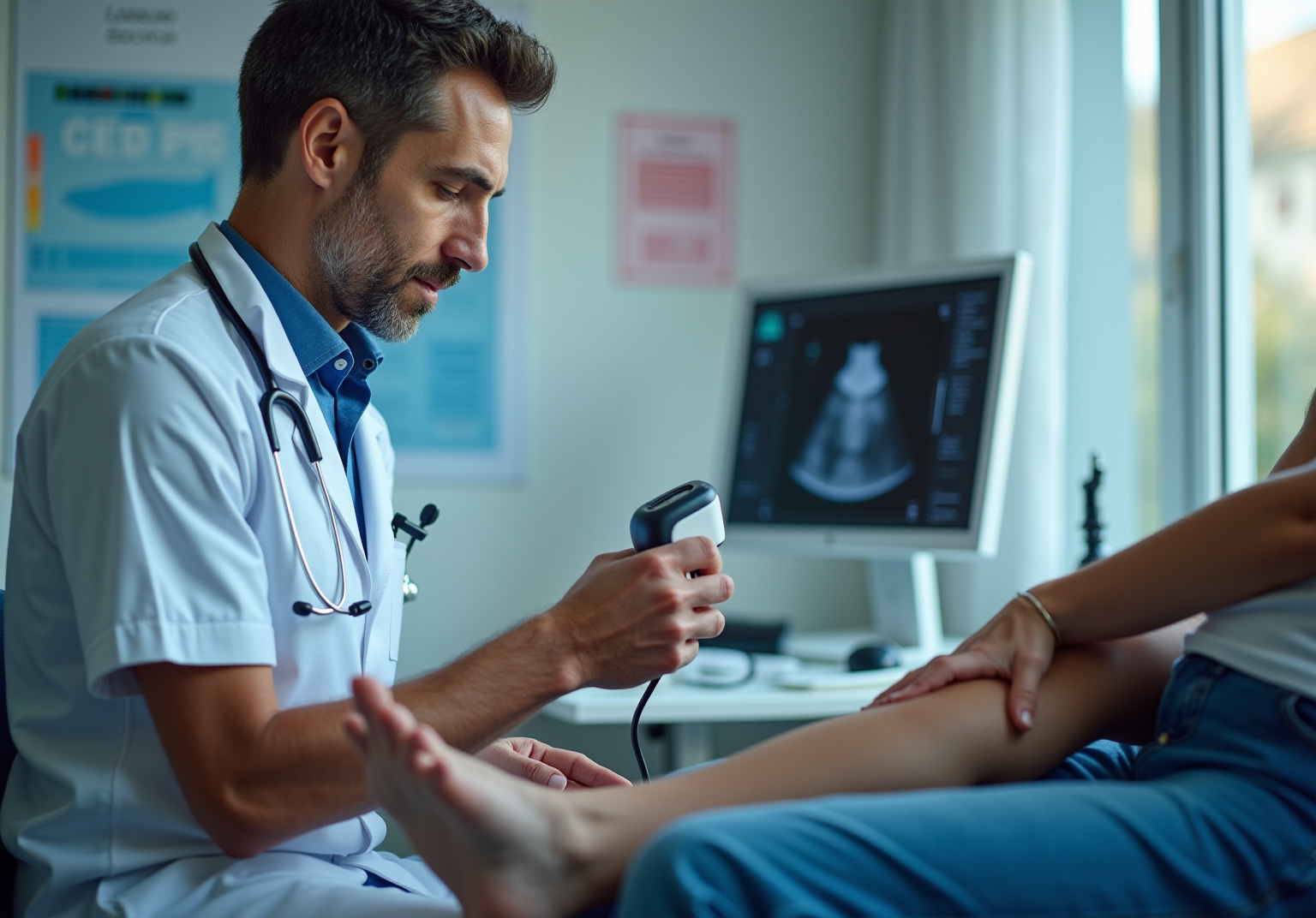
In addition to this, Amavita's offers a solution. With this advanced diagnostic tool, healthcare providers can conduct thorough right at the bedside. This enables early detection of complications related to , which is vital for . Powered by AISAP's FDA-approved AI ultrasound platform, allows for real-time analysis of heart structure and function, significantly enhancing cardiovascular care for those living with .
Furthermore, considering that 25% of rely on post-acute care facilities, the ability to identify and address cardiovascular issues early is essential. It can make a real difference in reducing readmissions and improving overall patient outcomes. If you or a loved one are experiencing symptoms, don’t hesitate to reach out for support. You deserve the best care possible.

Identify Causes and Risk Factors of PAD
often results from atherosclerosis, a condition in which plaque builds up in the arteries. Understanding the can empower you to take charge of your health. Here are some key contributors:
- Age: As we age, particularly after 50, the risk of PAD increases. Studies show that around 14.5% of those over 70 and nearly 60% of individuals over 85 are affected by PAD.
- Smoking: Tobacco use significantly raises the risk. Smokers are much more likely to develop PAD than non-smokers. Quitting smoking is a vital step toward reducing this risk.
- Diabetes: If you have diabetes, your chances of developing PAD can be up to four times higher. This condition can lead to vascular damage and more plaque formation.
- High Blood Pressure and Cholesterol: Both can harm your arteries, increasing the likelihood of PAD. Regular monitoring and management are crucial.
- Family History: A family history of cardiovascular diseases can heighten your risk for PAD, making it important to be aware of your family's health background.
- Sedentary Lifestyle: Not being active can worsen other , so incorporating regular exercise is essential for maintaining .
Recognizing these allows you to make informed lifestyle choices that may help reduce your risk of developing PAD. At Amavita Heart and ®, we prioritize and for your circulatory health. Did you know that about 6.5 million people aged 40 and older in the United States are living with PAD? Alarmingly, 70% of cases of PAD show no symptoms, which is why is so important.
Our specialists use to identify blockages and offer expert treatment options, including and Varithena treatment. These options aim to restore blood flow, ensuring you receive the care necessary to enhance your mobility and quality of life. Remember, you’re not alone in this journey; we’re here to support you every step of the way.

Recognize Symptoms of PAD
Symptoms of pad can show up in various ways, and it’s important to pay attention to them. Here are some common indicators:
- Claudication: This involves , which usually eases with rest. Many elderly patients experience claudication, making it a key symptom to watch for.
- : You might notice weakness or numbness in your lower limbs when you exert yourself. This can be concerning and deserves further investigation.
- : If you feel a noticeable difference in temperature between one leg and the other, it could indicate reduced blood flow.
- on your toes, feet, or legs are serious signs of advanced pad and require immediate medical attention.
- : If your affected leg appears pale or bluish, it may reflect compromised circulation.
early is crucial. Timely intervention can significantly improve management and outcomes for individuals with pad . emphasize that being aware of these signs can empower you to , ultimately enhancing your . Remember, you’re not alone in this journey, and reaching out for support is a strong step towards better health.

Explore Diagnosis and Testing for PAD
Diagnosing at Amavita is a compassionate journey that combines thorough physical examinations with tailored diagnostic tests, especially for those at higher risk.
- : This simple yet effective test compares blood pressure readings from your ankle and arm, offering a quick glimpse into your blood flow. If your ABI value is below 0.9, it indicates , while values between 0.9 and 1.0 suggest a borderline condition that may require further evaluation. Notably, leading cardiovascular organizations recommend measuring ABI for every smoker over 50, every diabetic over 50, and all individuals over 70.
- Ultrasound: This , helping to identify any blockages in your arteries. It’s particularly useful for assessing the severity of and guiding treatment options, ensuring you receive focused tailored to your needs.
- Angiography: In some cases, we may need to use imaging tests with contrast dye to get a detailed view of your arteries. This advanced imaging capability at Amavita underscores our commitment to comprehensive cardiovascular evaluations.
- : These are crucial for identifying risk factors like high cholesterol and diabetes, which can contribute to the progression of .
Understanding these is vital for you, as it prepares you for your medical appointments and encourages open conversations with your healthcare providers. Did you know that nearly 50% of individuals with PAD don’t show any symptoms? This highlights the , especially for those over 50 or with risk factors like smoking and diabetes.
Recent , such as the estimated toe-brachial index (eTBI), provide faster, more accurate assessments for , enhancing early detection and treatment options. Approximately 30% of individuals diagnosed with may require , highlighting the importance of accurate diagnosis and the personalized care that Amavita is proud to offer. Remember, you’re not alone in this journey; we’re here to support you every step of the way.

Review Treatment Options for PAD
Managing pad effectively is all about easing your symptoms and preventing complications. Let’s explore some key that can make a real difference in your life:
- Lifestyle Changes: Quitting smoking, embracing a , and staying active can significantly improve your symptoms and overall vascular health. Did you know that in individuals with PAD, especially if you also have diabetes or hypertension? Making these changes can truly enhance your well-being.
- Medications: Doctors often prescribe antiplatelet agents like aspirin, along with medications to help . These medications are vital for preventing clotting and , which is essential for managing pad . At Amavita, we also understand that medication costs can be a concern; for mild PAD cases, expenses can range from $50 to $300 per month without insurance. We’re here to help you navigate those financial choices.
- Supervised Exercise Therapy: and reduce symptoms in individuals with pad . Many people who participate in these programs report feeling more mobile and enjoying a better quality of life. Isn’t it encouraging to know that movement can lead to such positive changes?
- : Techniques like , allowing for quicker recovery times and less discomfort compared to traditional surgery. At Amavita, we utilize advanced imaging and drug-coated balloons, which have shown promise in keeping arteries open after procedures. This means less time in the hospital and a faster return to your daily activities.
- Surgery: In more severe cases, bypass surgery might be necessary to restore adequate blood flow. It’s important to discuss all your with your healthcare provider, especially since surgical interventions for severe pad can cost between $20,000 and $70,000 or more.
By understanding these , you can work together with your healthcare providers at Amavita to create a that meets your specific needs. Remember, you’re not alone in this journey; we’re here to support you every step of the way.

Conclusion
Understanding Peripheral Artery Disease (PAD) is crucial for anyone wanting to enhance their vascular health and overall well-being. This circulatory condition, primarily caused by atherosclerosis, affects millions, particularly those over 50. By recognizing the symptoms, understanding the risk factors, and knowing the available treatment options, you can take charge of your health and seek timely medical help.
Throughout this article, we’ve explored key points, including:
- What PAD is and how common it is
- The various causes and risk factors like age, smoking, and diabetes
- The symptoms that may signal this condition
- Diagnostic methods such as the Ankle-Brachial Index (ABI) and ultrasound, which are vital for early detection
- Treatment options ranging from lifestyle changes and medications to minimally invasive procedures and surgical interventions
Ultimately, managing PAD requires a proactive approach to your health. By staying informed about this condition and its implications, you can make empowered choices that lead to better outcomes. Have you considered taking the first step towards seeking help and adopting healthier habits? Doing so can significantly enhance your quality of life and lower the risk of severe complications.
Regular screenings and consultations with healthcare providers are essential. They play a crucial role in navigating the complexities of PAD management. Remember, you’re not alone in this journey; support is available, and taking action now can lead to a healthier future.
Frequently Asked Questions
What is Peripheral Artery Disease (PAD)?
Peripheral Artery Disease (PAD) is a common circulatory condition that primarily affects the legs, occurring when arteries narrow due to atherosclerosis, which involves fatty deposits building up on artery walls. This leads to reduced blood flow and can result in discomfort like leg pain or cramping during physical activities.
How many people in the United States are affected by PAD?
Over 12 million individuals in the United States are living with Peripheral Artery Disease (PAD), making it a significant chronic health issue.
What are the complications associated with PAD?
PAD can lead to serious complications, including a heightened risk of heart attack and stroke, which makes understanding and managing the condition crucial.
What is Amavita's CardioElite™ and how does it relate to PAD?
Amavita's CardioElite™ is an advanced diagnostic tool that enables healthcare providers to conduct thorough cardiac assessments at the bedside. It facilitates early detection of complications related to PAD, which is vital for improving patient outcomes.
What factors increase the risk of developing PAD?
Key risk factors for developing PAD include: - Age (risk increases after 50) - Smoking (significantly raises the risk) - Diabetes (can increase risk up to four times) - High blood pressure and cholesterol - Family history of cardiovascular diseases - Sedentary lifestyle
How prevalent is PAD among older adults?
Studies show that around 14.5% of individuals over 70 and nearly 60% of those over 85 are affected by PAD.
Why is proactive screening for PAD important?
About 70% of PAD cases show no symptoms, making proactive screening essential for early detection and management of the condition.
What treatment options are available for PAD?
Treatment options for PAD include advanced diagnostic imaging to identify blockages and minimally invasive procedures like venous ablation and Varithena treatment, which aim to restore blood flow and enhance mobility and quality of life.
List of Sources
- Define Peripheral Artery Disease (PAD)
- New roadmap to lower the risk of amputation in peripheral artery disease (https://heart.org/en/news/2024/05/14/new-roadmap-to-lower-the-risk-of-amputation-in-peripheral-artery-disease)
- news.cuanschutz.edu (https://news.cuanschutz.edu/department-of-medicine/research-semaglutide-patients-peripheral-artery-disease-diabetes)
- Patient perspectives on peripheral artery disease education and an online peripheral artery disease video education tool (https://sciencedirect.com/science/article/pii/S2949912725000200)
- Vascular surgery provides patients with new minimally invasive treatment for peripheral artery disease (https://health.ucdavis.edu/news/headlines/vascular-surgery-provides-patients-with-new-minimally-invasive-treatment-for-peripheral-artery-disease-/2025/05)
- Identify Causes and Risk Factors of PAD
- About Peripheral Arterial Disease (PAD) (https://cdc.gov/heart-disease/about/peripheral-arterial-disease.html)
- Prevalence of Peripheral Arterial Disease and Principal Associated Risk Factors in Patients with Type 2 Diabetes Mellitus: The IDON-Peripheral Arterial Disease Study | MDPI (https://mdpi.com/2673-4540/5/2/15)
- Intermountain Health Study Finds Peripheral Artery Disease Often Underdiagnosed & Undertreated; Opportunity to Improve Treatments (https://news.intermountainhealth.org/new-study-finds-peripheral-artery-disease-often-underdiagnosed-and-undertreated-opportunity-to-improve-treatments-lower-death-rates)
- aging-us.com (https://aging-us.com/news-room/long-lived-families-show-lower-risk-for-peripheral-artery-disease)
- Recognize Symptoms of PAD
- heart.org (https://heart.org/en/news/2025/09/30/is-your-leg-pain-actually-pad-watch-for-these-warning-signs)
- aafp.org (https://aafp.org/pubs/afp/issues/2019/0315/p362.html)
- michiganmedicine.org (https://michiganmedicine.org/health-lab/peripheral-artery-disease-what-know)
- New study finds Peripheral Artery Disease often underdiagnosed and undertreated (https://abc4.com/community/intermountainhealthcare/new-study-finds-peripheral-artery-disease-often-underdiagnosed-and-undertreated)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S1078588415009235)
- Explore Diagnosis and Testing for PAD
- news-medical.net (https://news-medical.net/news/20250710/Improving-early-detection-of-peripheral-artery-disease-with-a-new-diagnostic-method.aspx)
- Ankle-brachial index - Mayo Clinic (https://mayoclinic.org/tests-procedures/ankle-brachial-index/about/pac-20392934)
- Study finds high rates of undiagnosed and untreated peripheral artery disease (https://news-medical.net/news/20250331/Study-finds-high-rates-of-undiagnosed-and-untreated-peripheral-artery-disease.aspx)
- Breaking the Bottleneck: How PAD Diagnostic Testing Transforms Patient Care and Healthcare Revenue (https://newman-medical.com/breaking-the-bottleneck-how-pad-diagnostic-testing-transforms-patient-care-and-healthcare-revenue)
- Ankle Brachial Index (https://med.stanford.edu/stanfordmedicine25/the25/ankle-brachial-index.html)
- Review Treatment Options for PAD
- New Treatments for PAD (2025) (https://cacvi.org/new-treatments-for-pad)
- The Latest Treatments for Peripheral Artery Disease (PAD) | Washington Vascular (https://washingtonvascular.com/the-latest-treatments-for-peripheral-artery-disease-pad)
- First in the World: LVHN Performs Procedure Offering New Hope to Patients Living with Peripheral Artery Disease (PAD) (https://lvhn.org/news/first-world-lvhn-performs-procedure-offering-new-hope-patients-living-peripheral-artery)
- Vascular surgery provides patients with new minimally invasive treatment for peripheral artery disease (https://health.ucdavis.edu/news/headlines/vascular-surgery-provides-patients-with-new-minimally-invasive-treatment-for-peripheral-artery-disease-/2025/05)
- 5 New Treatments for Peripheral Artery Disease - Pittsburgh Vascular Specialists (https://greaterpittsburghvascular.com/2024/10/23/5-new-treatments-for-peripheral-artery-disease)